Research Bio
Daniela Kaufer is a Professor of Integrative Biology and Neuroscience. Her lab investigates how the brain responds to perturbations such as stress and brain injury, focusing on the mechanisms underlying resilience and vulnerability throughout life and aging. They aim to uncover the foundations of human mental health and neurological diseases, including PTSD, depression, epilepsy, and age-related dementia, while exploring new treatments and preventive measures. Additionally, they study the biological effects of psychedelic drugs on the brain and the complex interactions between stress, psychedelics, and neurobiology. Their research combines cutting-edge neuroscience with artificial intelligence to enhance our understanding of resilience and develop innovative approaches to improve mental health and neurological outcomes.
Research Expertise and Interest
neuroscience, aging, dementia, stress, epilepsy, traumatic brain injury, blood brain barrier, resilience, trauma, psychedelics, glia, myelin
In the News
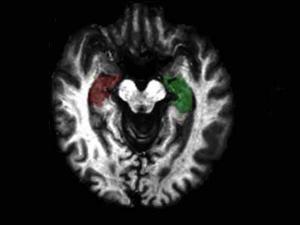
Anxiety and PTSD Linked to Increased Myelin in Brain
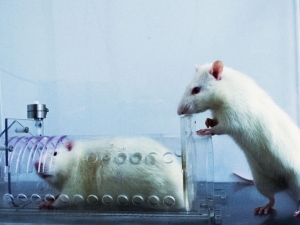
Rats prefer to help their own kind. Humans may be similarly wired
Drugs that quell brain inflammation reverse dementia
Bromances may be good for men’s health
Male friendships, portrayed and often winked at in bromance movies, could have healthful effects similar to those seen in romantic relationships, especially when dealing with stress.
Blocking Hormone Could Eliminate Stress-Induced Infertility
Berkeley scientists show that the effects of chronic stress on fertility persist long after the stress is gone.
Commonly available blood-pressure drug prevents epilepsy after brain injury
UC Berkeley neuroscientist Daniela Kaufer and colleagues in Israel and Germany have shown in rats that a drug commonly prescribed for hypertension can nearly eliminate the epilepsy that often follows severe head injury. Nearly one in five cases of epilepsy is the result of head trauma.
Seizing Control of Brain Seizures
Daniela Kaufer made a startling discovery about the effect of psychological stress on the brain a few years after serving in the Israeli army during the first Gulf War.
New evidence that chronic stress predisposes brain to mental illness
University of California, Berkeley, researchers have shown that chronic stress generates long-term changes in the brain that may explain why people suffering chronic stress are prone to mental problems such as anxiety and mood disorders later in life.
Five new Bakar Fellows pursue path to marketplace
Five UC Berkeley scientists eager to take their lab-bench discoveries into the marketplace have been awarded Bakar Fellowships to help them achieve their goals.
Researchers find out why some stress is good for you
New research by Kaufer and UC Berkeley post-doctoral fellow Elizabeth Kirby has uncovered exactly how acute stress – short-lived, not chronic – primes the brain for improved performance.
New neurons help us to remember fear
UC Berkeley’s Daniela Kaufer and colleagues have discovered one way by which emotions such as fear affect memory. The brain’s emotional center, the amygdala, induces the hippocampus, a relay hub for memory, to generate new neurons. In a fearful situation, these newborn neurons are activated by the amygdala, providing a “blank slate” for the new fearful memory.
Featured in the Media
Drugs that reduce inflammation in the brain may be able to slow or reverse age-related dementia, a team of Berkeley researchers has found. The work promises not only potential treatments for cognitive decline but also surprising new insights into what causes dementia. "I think we're showing a new way to explain very early stages of decline in the brain, and some of it, interestingly, is decline in the normal aging brain, and that's something that we really know very, very little about, or that we knew almost nothing about before we looked at it," says integrative biology professor Daniela Kaufer, the study's senior author. "We're offering a new way to look at it, and the answer came from sort of an unexpected angle. You would think that it would be the cells -- the neurons, the nerve cells, but actually the real secret was in the blood vessels in the brain. ... What we found is dysfunction of the blood-brain barrier that increases in age, and we documented it in rodents and in humans." Link to audio. For more on this, see our press release at Berkeley News. Other stories on this topic appeared in the Daily Mail (UK), Technology.org, New Atlas, MindBodyGreen, and Henri Le Chat Noir.
Teaching
Special Study in Integrative Biology [INTEGBI 298 - 250]
Graduate Research [INTEGBI 299 - 250]
Neuroscience Graduate Research [NEU 292 - 019]
Neuroscience Research Review [NEU 295 - 016]
Special Study in Integrative Biology [INTEGBI 298 - 210]
Graduate Research [INTEGBI 299 - 210]
Integrative Human Biology [INTEGBI 77A - 001]
The Neurobiology of Stress and Resilience [INTEGBI C139 - 001]
Neuroscience Graduate Research [NEU 292 - 019]
Neuroscience Research Review [NEU 295 - 016]
The Neurobiology of Stress and Resilience [NEU C166 - 001]
Special Study in Integrative Biology [INTEGBI 298 - 210]
Graduate Research [INTEGBI 299 - 210]
Neuroscience Graduate Research [NEU 292 - 019]
Neuroscience Research Review [NEU 295 - 016]